|
The effects of dapagliflozin on glycaemic parameters, bodyweight and BP in large clinical trials in patients with T2D are summarized in Sect. A modest decrease in blood pressure (BP) was also seen with dapagliflozin, which may be explained by a decrease in circulating volume because of the diuretic/natriuretic properties of the drug. The loss in bodyweight with SGLT2 inhibitors is less than that calculated from calorie loss due to glucuresis, which may be because of compensatory mechanisms such as increased energy intake. Dapagliflozin-induced glucuresis in patients with T2D was associated with caloric loss and a modest reduction in bodyweight, as well as mild osmotic diuresis and transient natriuresis. Urinary glucose excretion (glucuresis) was seen after the first dose of dapagliflozin, was continuous during the 24 h dosing interval and maintained over the course of therapy. 
Dapagliflozin increased the amount of glucose excreted in the urine and improved both fasting (FPG) and post-prandial plasma glucose levels in patients with T2D. Dapagliflozin is also available as fixed-dose dapagliflozin/metformin (Xigduo ®) and dapagliflozin/saxagliptin (Qtern ®) tablets.ĭapagliflozin is a highly potent (inhibitory constant 0.55 nmol/L) and reversible SGLT2 inhibitor that is > 1400 times more selective for SGLT2 than SGLT1, the main transporter responsible for glucose absorption in the gut. This article, written from an EU perspective, focuses on recent trials, including the large DECLARE-TIMI 58 cardiovascular (CV) outcomes trial in patients with T2D with or without established cardiovascular disease (CVD). The pharmacological properties and clinical use of dapagliflozin in adults with T2D have been extensively reviewed previously in Drugs. Dapagliflozin (Forxiga ®) is one such SGLT2 inhibitor that is approved for the treatment of T2D in various countries worldwide, including the EU and USA. This unique mechanism of action of SGLT2 inhibitors complements that of other classes of AHAs, allowing for their use as combination therapy with other AHAs, including insulin. These agents reduce reabsorption of glucose in the kidneys and facilitate its excretion in the urine by inhibiting the high-capacity glucose transporter SGLT2 located in the proximal convoluted tubule, thereby lowering glucose levels independently of insulin action. Sodium-glucose cotransporter-2 (SGLT2) inhibitors are a relatively new class of antihyperglycaemic agents (AHAs) for the treatment of type 2 diabetes (T2D). Given its antihyperglycaemic, cardioprotective and possibly renoprotective properties and generally favourable tolerability profile, dapagliflozin provides an important option for the management of a broad patient population, regardless of the history of CVD. 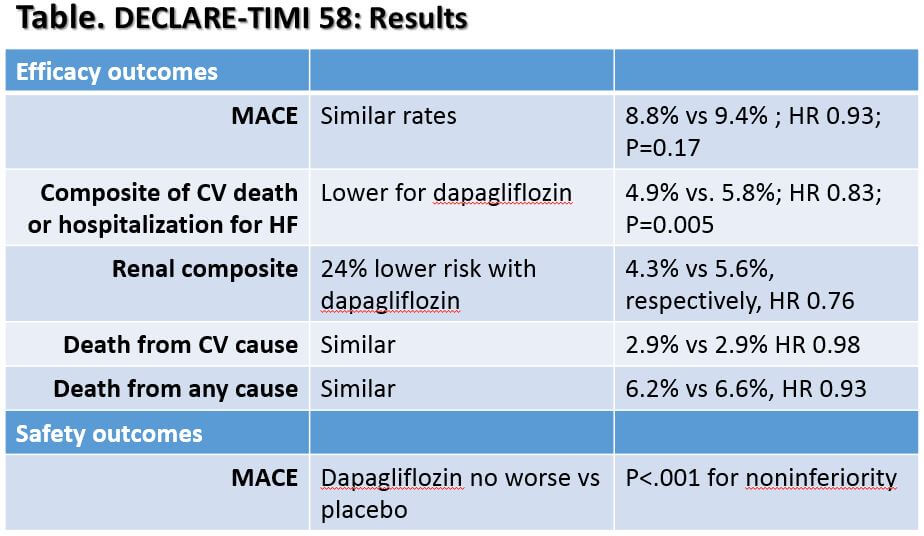 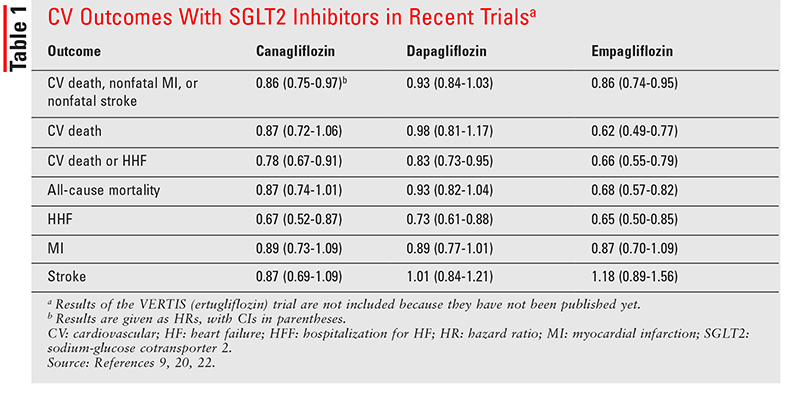
Dapagliflozin was generally well tolerated, with a low risk of hypoglycaemia diabetic ketoacidosis (DKA), although rare, and genital infections were more common with dapagliflozin than placebo. Dapagliflozin reduced the rate of cardiovascular (CV) death or hospitalization for heart failure (HHF), did not adversely affect major adverse CV events (MACE) and possibly reduced progression of renal disease relative to placebo in patients with established atherosclerotic CV disease (CVD) or multiple risk factors for CVD. In numerous well-designed clinical studies and their extensions, dapagliflozin as monotherapy and combination therapy with other antihyperglycaemic agents provided effective glycaemic control and reduced bodyweight and blood pressure (BP) across a broad spectrum of patients. In the EU, oral dapagliflozin once daily is approved for use as monotherapy (in patients who are intolerant of metformin) and as add-on combination therapy (with other glucose-lowering agents, including insulin) for T2D when diet and exercise alone do not provide adequate glycaemic control. Dapagliflozin (Forxiga ®) is a highly potent, reversible and selective sodium-glucose cotransporter-2 inhibitor indicated worldwide for the treatment of type 2 diabetes (T2D).
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
